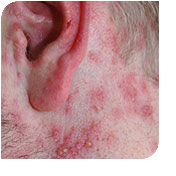
 Post Herpetic Neuralgia (Pain from Shingles)
Post Herpetic Neuralgia (Pain from Shingles)
The shingles is a reactivation of the chicken pox (also known as varicella-zoster) which occurs in the distribution of usually one, but sometimes more than one, peripheral nerve. It begins with a red rash that eventually causes vesicular (fluid filled) lesions and it is very painful. When this occurs, in general, the patient should be treated with a medications that works against the virus itself such as acyclovir (Zovirax), famciclovir (Famvir), or valacyclovir (Valtrex). The duration of the vesicles is usually one to two weeks. The shingles usually reactivates when the body is being affected by another stress such as an illness, surgery, or cancer. Usually the pain subsides when the skin lesions heal.
Unfortunately, for 10-20% of all patients who get the shingles, the pain does not subside. When the pain persists long (one month by some authors, 3 months by others) after the vesicles are healed, this is called a post-herpetic neuralgia. The chance of having a post-herpetic neuralgia increases with increasing age and is in about 60% of those patients who are over 60. The natural history of this disease is to improve and only a small percentage of patients with this disease have persisting pain greater than one year.
Treating Post-Herpetic Neuralgia (PHN)
The only FDA approved treatments for this condition are Neurontin, Lyrica an anti-epileptic drug (AED), Lidoderm, a topical lidocaine preparation, and Qutenza, a prescription strength, capsacin patch applied in the physician's office. Qutenza is applied in the physicians office and if you get a benefit, it typically lasts for more than 3 months. Since there is very little systemic absorption of capsacin, there are minimal side effects and no significant drug interactions.
Lidoderm is applied for sixteen hours to the affected area and removed for eight hours. Unfortunately, sometimes the location or size of the area make it impossible or impractical to use the Lidoderm. In addition, some patients do not get sufficiently long relief of pain during the eight hours the patch has to be removed each day.
Neurontin has been demonstrated in two placebo controlled trials to be effective in decreasing the pain of post-herpetic neuralgia. The medication is extremely safe and well tolerated. When Neurontin® is not successful, then other AEDs should be tried as the response to one medication does not predict a response to the others. Lyrica works in a manner similar to Neurontin but has better absorption.
Cymbalta® is commonly used for all neuropathic pain even though it is only approved for one particular form of neuropathic pain.
Other commonly used AEDs for post-herpetic neuralgia include Trileptal, Tegretol, Keppra, and Zonisamide. Additional medications used for post-herpetic neuralgia include the tricyclic antidepressants such as Elavil (amitriptyline) or Pamelor (nortriptyline). These medications, however, sometimes cause too many side effects including weight gain, constipation, and sleepiness. In addition, these medications are usually not recommended for patients over the age of 65 due to an increased risk of falls.
Zostavax - The Shingles Vaccine
There is now a vaccine to help prevent one from getting the shingles. The vaccine is recommended for those who are over the age of 60 who are not immunosuppressed. The vaccine is safe for those over the age of 50. The vaccine prevents about ½ of the cases of the shingles. It prevents about 2/3rds of the most severe cases of post-herpetic neuralgia.
The vaccine for Varicella Zoster has been one of the most exciting developments in the neuropathic pain field. This vaccine essentially prevents the development of shingles by boosting the body's immune system to the Zoster virus. The shingles represents a reoccurence of the herpes zoster virus or chicken pox virus which was not completely eradicated during childhood. The occurance rate increases as one gets older therefore, a study of people older than 60 was conducducted and participants received either the varicella zoster vaccine (VZV) or a placebo. Subjects were followed an average of 3.12 years.
The placebo group gave insight into the natural history of the shingles. The chance of getting shingles was found to be about 1.1% each year. Those over 70 were only about 10% more likely to get shingles than those between 60 and 70. A total of 642 subjects in the placebo group got the shingles. Unlike traditional care, all of these patients were instructed what to look for in case they got a rash. They were quickly seen and started on Famvir. Because of this prompt treatment, the incidence of post-herpetic neuralgia was extremely low. Post-herpetic neuralgia is typically defined as pain beyond 90 days which was only 80 of the initial 642 patients or about 12%. This is much less than one would expect and probably represents early treatment with Famvir. Of note, only 33 patients had pain 6 months after the initial outbreak so the effect of the Famvir appears to be to prevent 95% of long term post-herpetic neuralgia.
The group that received the vaccine did even better than the placebo group. The chance of getting the shingles was less than 1/2 of the placebo group or about 1 patient per every 200 vaccinated individuals. The vaccine appears to be more effective in the 60-69 year old group (65% effective) versus those over the age of 70 (55% effective). Just as impressive, of the 315 patients in the vaccine group who developed the shingles, only 27 (9%) developed post-herpetic neuralgia and only 9 (3%) had long term (> 6 months) of post-herpetic neuralgia. Therefore, not only did the vaccine prevent a high percentage of cases of post-herpetic neuralgia, those who did get the shingles were less likely to develop painful complications.
*The information for this article is from the New
England Journal of Medicine article "A Vaccine to Prevent Herpes Zoster
and Postherpetic Neuralgia in Older Adults" N Engl J Med 352:22 pp. 2271-2284.



